WFPI in Malawi - and Imaging the World in Uganda/Malawi
Project identified by Drs. Savvas Andronikou, Arthur Daire (Blantyre), Peter Maseko (Salima) and Kristen DeStigter (Imaging the World)
[Nov 2015 update on this project: scroll down]
In July 2014 WFPI undertook an exploratory outreach mission to teach and determine pediatric radiology needs in different environments in Malawi. The visit aimed to provide tele-reading support for pediatric imaging and pave the way for future teaching and training visits.
Dr. Tracy Kilborn (Head of Pediatric Imaging, Red Cross War Memorial Children’s Hospital, Cape Town) volunteered for the trip. A member of the South African Pediatric Imaging Society and a WFPI tele-reading volunteer, Dr. Kilborn's geographical proximity and experience with endemic diseases, equipment constraints and environmental limitations leave her well equipped for regional outreach.
The trip covered 4 different health facilities in Malawi
- Queen Elizabeth Hospital, Blantyre
- Chiradzulu District Hospital - MSF AIDS-HIV project
- Kamuzu Central Hospital, Lilongwe
- Pothawira Haven, Salima
Dr. Tracy Kilborn with Dr. Peter Maseko, Pothawaria Haven Salima, Malawi

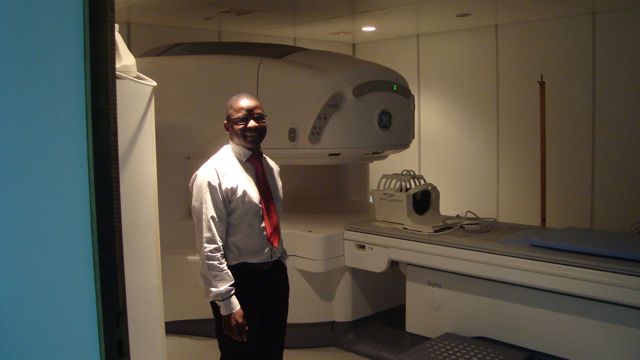 Queen Elizabeth Hospital Blantrye offers 300 Pediatric beds and conducts 100,000 Pediatric reviews per year in A/E with 20,000 Pediatric admissions per year. A 0.75T open magnet, installed by Johns Hopkins as a research magnet, is used by the hospital. A CT machine purchased 4 years ago is in storage while waiting for a room to be built. The sole MoH radiologist is stretched to support radiography and ultrasound as well as MRI.
Queen Elizabeth Hospital Blantrye offers 300 Pediatric beds and conducts 100,000 Pediatric reviews per year in A/E with 20,000 Pediatric admissions per year. A 0.75T open magnet, installed by Johns Hopkins as a research magnet, is used by the hospital. A CT machine purchased 4 years ago is in storage while waiting for a room to be built. The sole MoH radiologist is stretched to support radiography and ultrasound as well as MRI. Right: Dr Arthur Dale, MoH radiologist, Queen Elizabth Hospital Blantyre
Below: Paediatric Ward, Queen Elisabeth Hospital, Blantyre


Teaching activities in Blantyre and at Kamauzu Central Hospital in Lilongwe included lectures to the paediatric and paediatric surgical staff on:
- Approach to a paediatric CXR,
- Approach to a paediatric AXR,
- Imaging of neonatal GI emergencies,
- Imaging of non-accidental injuries,
- Basic approach to nuclear medicine in renal disorders
along with teaching paediatric ultrasound techniques to sonographers, consultations on complex medical and surgical cases and engaging in discussions on CXR technique with radiographers.
Among the conclusions of the trip: Point of Care (PoC) ultrasound in all the facilities visited would be of immense relevance and value.
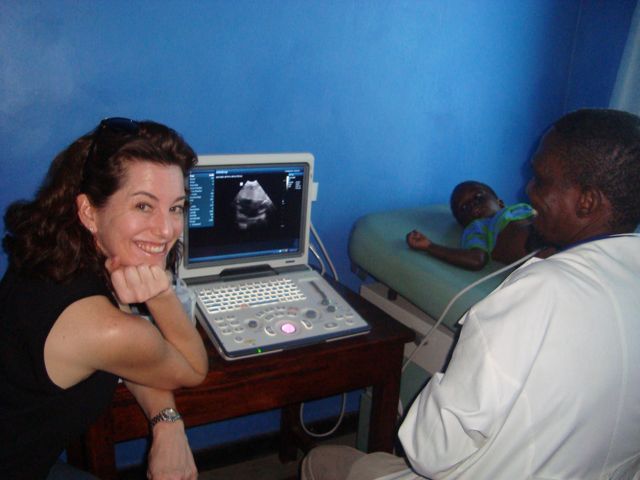
 At Pothawira Haven, Salima, Dr. Peter Maseko (image left), 4 nurses and an occasional volunteering medical student run a clinic that sees 200-300 patients a day. Pothawira also supports 110 orphans, all of whom live and are schooled at the Haven. The entire project is funded through donations, with Dr. Kay North and the Children's Mercy Hospital, Kansas, USA, leading the support. WFPI delivered a new portable ultrasound machine, donated to Pothawira by Dr. Kristen DeStiger of Imaging the World, in view of a future ITW/Kansas project in Malawi that WFPI hopes to partner with. Accompanied by a radiologist resident from Lilongwe, Dr. Pamela Gunde (image below) and with excited orphans queueing up as teaching material, the ultrasound training at the clinic began. After 2 days, the two physicians could competently scan pediatric heads, chests, abdomens and look for pericardial effusions. FOR AN UPDATE ON THIS PROJECT, NOV 2015, SEE BELOW
At Pothawira Haven, Salima, Dr. Peter Maseko (image left), 4 nurses and an occasional volunteering medical student run a clinic that sees 200-300 patients a day. Pothawira also supports 110 orphans, all of whom live and are schooled at the Haven. The entire project is funded through donations, with Dr. Kay North and the Children's Mercy Hospital, Kansas, USA, leading the support. WFPI delivered a new portable ultrasound machine, donated to Pothawira by Dr. Kristen DeStiger of Imaging the World, in view of a future ITW/Kansas project in Malawi that WFPI hopes to partner with. Accompanied by a radiologist resident from Lilongwe, Dr. Pamela Gunde (image below) and with excited orphans queueing up as teaching material, the ultrasound training at the clinic began. After 2 days, the two physicians could competently scan pediatric heads, chests, abdomens and look for pericardial effusions. FOR AN UPDATE ON THIS PROJECT, NOV 2015, SEE BELOW

WFPI is conducting research on volume sweep ultrasound for use in precisely this type of setting: see here
 Chiradzulu District Hospital, which may have a high prevalence of Childhood TB Chiradzulu District Hospital, which may have a high prevalence of Childhood TB
|

Happy volunteers for the ultrasound training...!
|

Kamuzu Central Hospital, Lilongwe
|
|

In November 2015 Dr. Kay North of the Children's Mercy Hospital, Kansas, and Imaging The World (below) visited Pothawira and Dr Maseko again.
Pothawira Clinic is funded by donations and Dr. Kay North leads the support
“Although it is a bit unconventional, we scanned patients prior to their evaluation with either Dr. Maseko, Dr. Alaniz, or the other clinical officer. Since most of the women traveled to the clinic specifically to be scanned, we found better patient flow when we could send them for evaluation with the Ultrasound results noted in their medical passports. However, we did not prescan the children, they were evaluated by Dr. Maseko first and if they required imaging, we worked them in as soon as possible.”We saw varying pathology. Renal stones with severe hydro, pelvic kidneys, cervical cancer grown into the bladder causing significant hydro, large thyroid mass compressing the airway, large ovarian masses, fibroid uterus, gall stones, inguinal hernias containing bowel...For more:.

WFPI is now looking to organize a follow up pediatric radiology support trip to Pothawira
|
.

.... in Malawi (see above) and Uganda: BELOW
WFPI partners with Imaging the World (ITW, www.imagingtheworld.org) so as to move pediatric PoC ultrasound forward in Uganda and Malawi.
 To date, ITW's work in Uganda has involved non-radiologists acquiring ultrasound images using anatomical landmarks on the skin and storing US sweeps as cine-loops in a standard format, to be read by radiologists at a distance (tele-reading).
To date, ITW's work in Uganda has involved non-radiologists acquiring ultrasound images using anatomical landmarks on the skin and storing US sweeps as cine-loops in a standard format, to be read by radiologists at a distance (tele-reading).
ITW has no pediatric protocols, so pediatric radiologist Dr. Julie Hurteau (Children's Hospital of Eastern Ontario, University of Ottawa, Canada) and Dr. Sabine Bélard (Charité University Hospital, Berlin, Germany) joined Dr. Kristen DeStigter (Fletcher Allen Health care, University of Vermont, Canada, and founder of Imaging the World) on Dr. DeStigter's trip to Uganda in August 2014. Dr. Bélard has been involved in WFPI's research on pediatric protocols for volume sweep ultrasound in Cape Town since 2013.
The aim: explore perspectives for establishing ultrasound as a diagnostic modality for pediatric pneumonia and tuberculosis in rural Uganda and set up some foundations for future ITW-WFPI collaboration in Malawi. UPDATE May 2015: protocols drafted, roll out all set, next visit being planned! More details soon!
Dr. Julie Hurteau with Sister Angela, the heart and soul of the rural health clinic of Nawanyago in Kamuli, and Dr. Kristen DeStigter.
.

A few figures for Uganda 
Uganda Population 2012 – 32.2 M
Expected population in 2020 – 44M
Ugandan population living in rural areas -84%
Total number of doctors in Uganda – 644
% of doctors in urban areas – 70%
Number of radiologists in Uganda – 34. This means that more than 80% of Ugandans (rural) have access to only 30% of the medically trained health care providers. Also they are seen at primary health care facilities which mostly lack any imaging facilities.
How about diseases in Uganda?
Acute respiratory infections - cause 15% of all deaths in children under five years of age
HIV prevalence - around 7%
Tuberculosis incidence - 175/100000 annually
Pediatric tuberculosis - up to 20% of the tuberculosis case load
Dr Bélard conducting a hands-on scanning session at the Mubende Regional Referral Hospital
Click here for more on Imaging the World